Building a provider network that meets adequacy standards is no small feat for healthcare organizations. As regulatory requirements evolve and patient needs diversify, ensuring beneficiaries have timely access to the right providers becomes increasingly complex. Organizations must navigate a maze of compliance benchmarks, analyze vast and often fragmented data, and address gaps across multiple specialties and service lines. Without the right tools and insights, maintaining an adequate network can quickly become a resource-intensive challenge, impacting both operational efficiency and the quality of care delivered.
In this blog we cover the common hurdles healthcare organizations face and how innovative solutions like the Milliman Network Optimizer can help streamline the path to network adequacy.
Specifically, we address the following questions:
1. What challenges do healthcare organizations face when trying to build, grow, and maintain a provider network that meets adequacy standards?
Building a strong network that meets adequacy standards is challenging for several reasons. One of the biggest hurdles is keeping up with complex and frequently changing regulatory requirements. Healthcare organizations also have to ensure there’s sufficient geographic and specialty coverage which becomes more difficult in the current environment of regional provider shortages. Additionally, plans are constantly managing data from multiple sources and making sure provider information is current and accurate. Balancing these factors—while managing costs and ensuring members have timely access to care—can be resource intensive. It’s a continuous process that requires significant coordination and strategic planning.
2. How does the Milliman Network Optimizer help overcome these challenges and strengthen provider networks?
Milliman developed the Network Optimizer to address key challenges faced by healthcare organizations. Organizations spend significant time and resources ensuring their networks meet regulatory requirements—specifically, that a percentage of beneficiaries are within the required distance or travel time to providers.
Milliman created a user-friendly tool that simplifies network adequacy analysis by integrating both proprietary claims data and public sources into an easy to use and interactive user-interface. With the Milliman Network Optimizer, healthcare organizations can easily evaluate network coverage for various specialties and service lines, quickly identify gaps, and adhere to regulatory requirements.
Figure 1 – The Milliman Network Optimizer
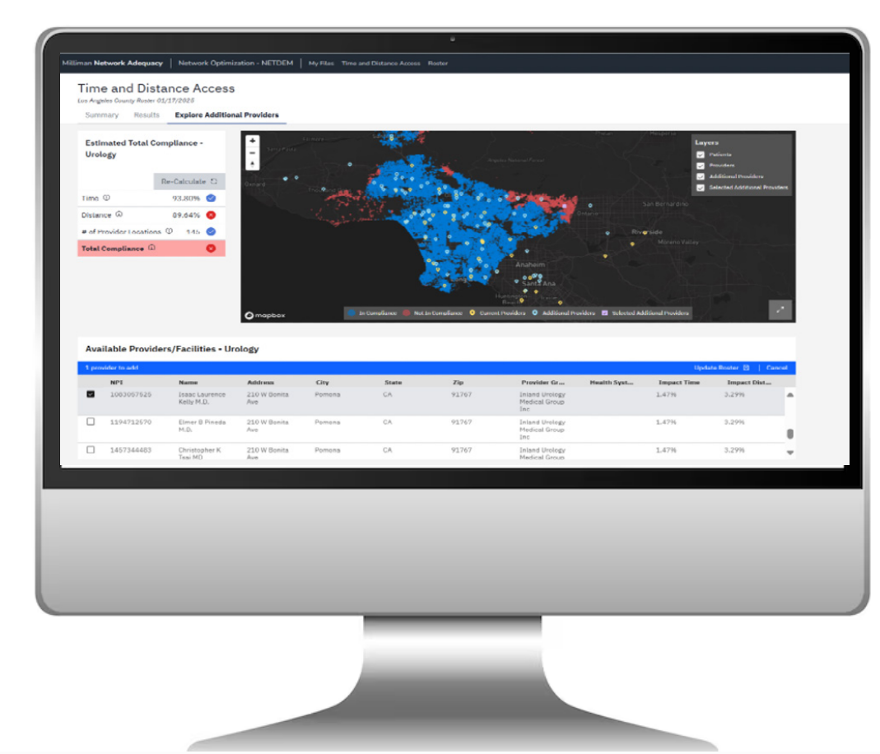
Beyond regulatory compliance, we designed the Network Optimizer to be an invaluable resource for strategic network design. The Network Optimizer is designed to support strategic decision making with respect to designing high performing networks and filling network access and adequacy gaps. The tool offers providers the resources to fill gaps and provides essential information about those providers such as affiliation with health systems, provider groups, quality scores, and contracting status with other payer networks.
3. What sets the Network Optimizer apart from other adequacy tools in the marketplace?
A key strength of the Network Optimizer is the data we leverage, including a world-class provider roster also known as the MedInsight Provider Registry, which powers the map interface and ensures we have accurate provider information. Maintaining a current provider list is a well-known challenge across the industry. Although plans may purchase lists, they often lack a truly accurate picture of the market. The reality is, there’s no single gold standard for physician rosters or registries, which makes this work especially important for network adequacy solutions.
At MedInsight, we’ve taken a rigorous approach by leveraging all the data available through Milliman and our emerging experience data. We curate an up-to-date provider list for each market—going beyond just standard credentials. For example, we don’t just rely on board certifications for service line assignments. If an internist’s claims data shows they primarily provide cardiovascular care, we’ll categorize them accordingly. Essentially, if a provider’s practice patterns reflect a certain specialty, our data-driven approach ensures they’re classified in the most meaningful way for network analysis.
4. What kinds of upgrades or improvements are you considering for the Network Optimizer?
Innovation with the Network Optimizer is propelled by our commitment to exploring adjacent use cases beyond its original design. Initially developed to evaluate regulatory compliance as health plans and networks evaluate options for expansion into new markets and lines of business, we have since expanded its capabilities to provide deeper insights into provider evaluation for network participation. We’re also excited to empower clients by enabling claims data integration for advanced disruption analysis, and by developing new features that further enhance network design and integrity. These ongoing enhancements reflect our dedication to delivering versatile solutions that address evolving market needs.
We’re actively engaging with our clients and prospective clients to understand their evolving needs. What makes this especially exciting is that the Network Optimizer leverages Milliman’s proprietary claims database, which isn’t available anywhere else. That unique data foundation gives us the ability to generate insights and solutions that truly set us apart.
Looking ahead, we have a roadmap that includes further development of our platform and integration of claims and other reference datasets. At the same time, we’re soliciting input from stakeholders about future use cases—because we see so much potential for innovation. It’s a dynamic process, and that collaborative approach is what makes this work so rewarding.
5. What resources are available to learn more about the Milliman Network Optimizer?
Schedule a call: Connect with one of our healthcare analytics experts.
Visit our website: Learn more about our Milliman Network Optimizer tool for ensuring network adequacy.
Watch the webinar: Register to attend our upcoming webinar “Optimizing provider networks: Strategies for access, compliance, and performance” and learn how to build strong, compliant provider networks.
